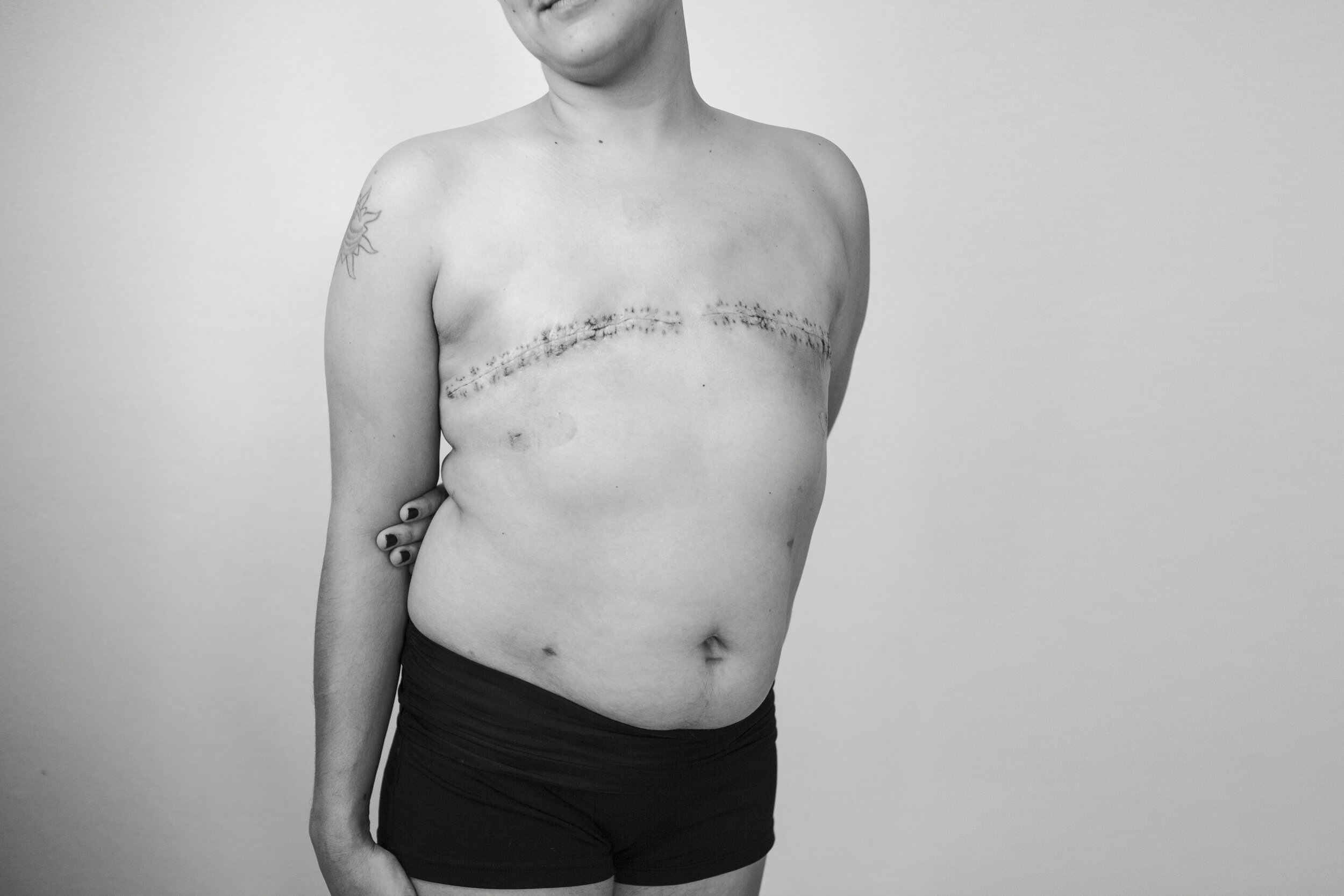
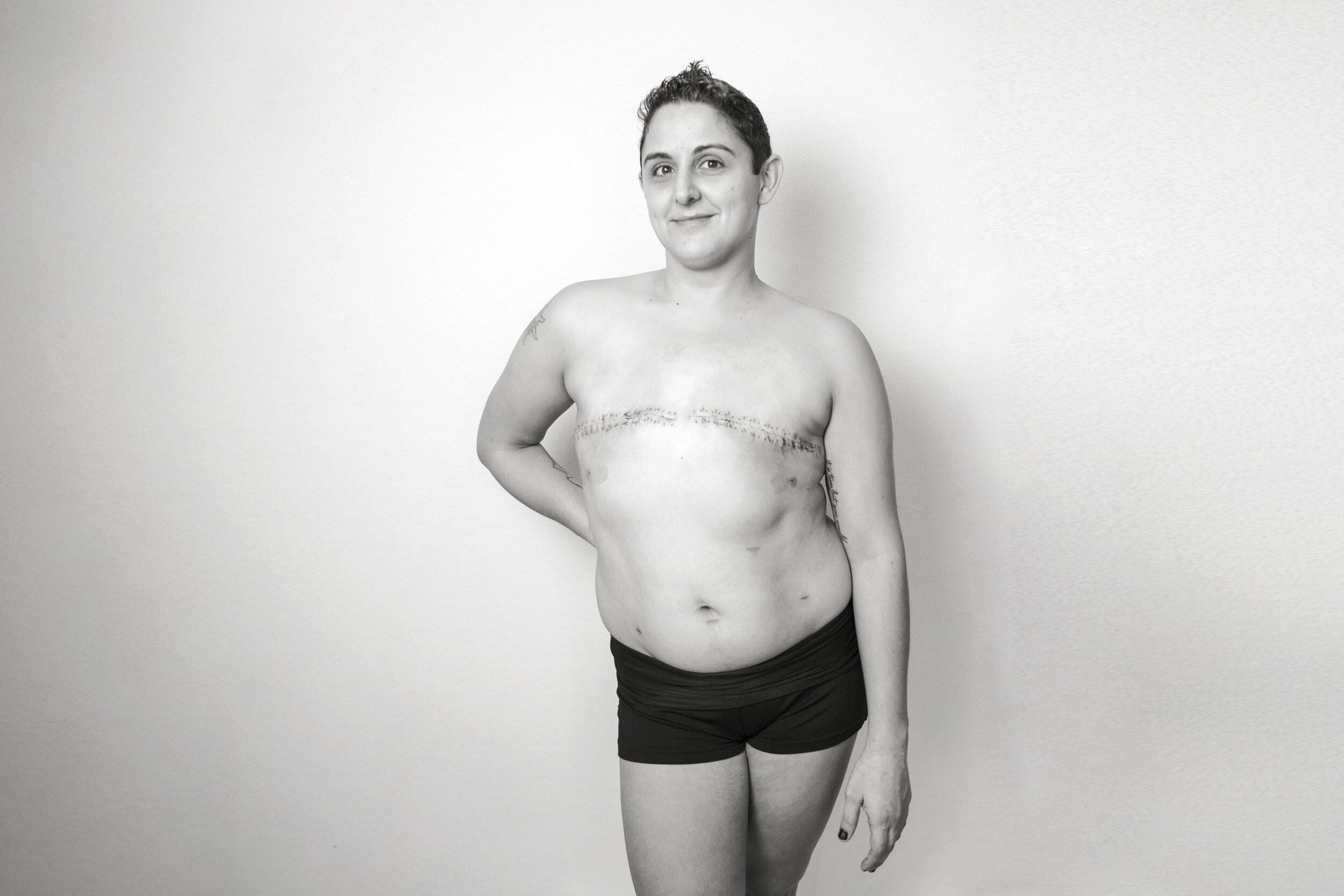
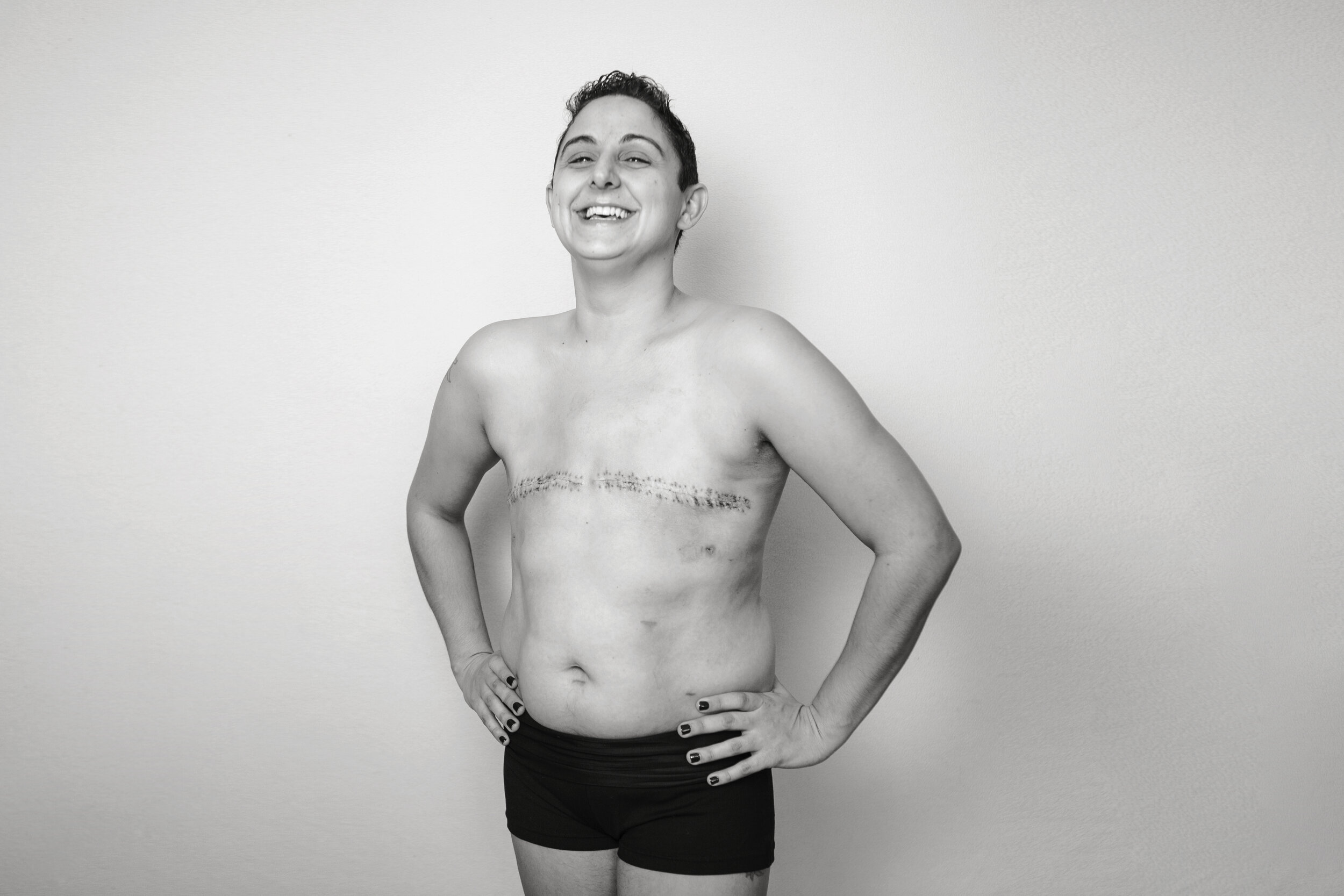
Anita Smithson (35 - she/her), Jack (7), Ava (5), and Will (1). You can view Anita’s original images from 2018 and 2016.
Minneapolis, MN
“I experienced one miscarriage in 2011. Jack was conceived within days of my estimated due date with my miscarried baby. My miscarriage was “ordinary”, early, and relatively easy from the physical aspects of it. It’s strange/lovely to me that Jack was conceived basically on my due date - had I carried that baby to term, I wouldn’t know Jack and it’s hard to imagine life without Jack. So - it was sad, but it also brought me a different baby to love eventually which makes the rainbow baby sweeter.
How has parenthood impacted your body image?
Parenthood has made me care so much less about what others think or judge about my body. It has made me a little bit more confident outwardly. But mostly, it’s made me more comfortable in who I am. That doesn’t always translate to confidence on the outside - but it does make me feel comfortable choosing clothing that feels good on my body, and being fully in my own body. Pregnancy, and giving birth, has made me appreciate my body more than previously. Strength that I did not know that I had. Our bodies are amazing.
What is your truth?
The more I have grown in myself, and learned to love myself - the more I trust my intuition. not just on what feels good and balanced/correct within my body and the abilities of my body - but also in my mind. Loving myself fully has allowed me to trust myself fully, which has made me a stronger, more courageous person.
Why did you choose to participate in this movement and share your story?
My last baby, William, just turned one. I am reflecting on his birth and our postpartum period. Last time I was with Ash in this space, I was thinking about having the delivery experience that I wanted. I didn’t get the entire experience that I thought I wanted (wanted a birth center delivery with a midwife; had a hospital induction 15 days overdue with a midwife but I did get my VBAC and had a very empowered delivery) but I am grateful for the birth education we participated in this time which helped me prioritize and find my footing in what was were my priorities and how to find those things no matter what circumstances put us in. My delivery of Will was an induction, starting at 42w with a Foley catheter. The next morning, it was removed and I was 5 cm but posterior. My midwife gave us the morning to go get breakfast, get a shower, and have a late morning pitocin induction. I was able to rest from about 10 am to 1 pm, when we called our Doula to have her come. By 1:30, I was in active labor and found myself retreating to my “cave” - a dark bathroom.
I had my husband and Doula run their hands lightly down my back while putting ice cold soaking wet towels on my back for each contraction. I hate being cold - so that I wanted this was so strange to me but it felt so wonderful and helped me stay cool through the very intense labor. By about 3:15, I had the urge to start pushing. My team was amazing, and I was able to push at the end of the bed in a squat, and then eventually moved to my side in bed to help Will turn. Delivering my VBAC baby was the most intense experience of my life. Physically, and emotionally. Will was born at 3:59 pm and was immediately brought to my chest. During labor I was focusing on growling low tones to help my body stay loose and it was like the opposite just burst out of me with his birth. I cried out “MY BABY! I DID IT! MY BABY!!” And then as soon as he started crying my body let out the remaining stress.
Having a provider that was using evidence based care, a Doula that was knowledgeable with VBAC and that I felt so comfortable with, having taken independent birthing education with my husband so he felt empowered and educated, and having a nurse who was comfortable with the birthing experience and able to assist our Doula and midwife in coaching me into good positioning and keeping my voice low were keys pieces to making it work.
Postpartum was really hard, though. I lost a decent amount of blood, and was very shaky. I was unable to stand up on my own for at least 12 hours after delivery and that was scary. I had horrible headaches, and all the staff at the hospital knew to do was test me for eclampsia - which I did not indicate as having. It’s was eventually my chiropractor who suggested I have my iron level tested, and I was very anemic. Getting on a good iron supplement made a huge difference in my well being but I only wish it had happened sooner. More impactful, though - was about 12 hours after Will’s birth - he started ‘throwing up’ and was having a hard time breathing. The special care nursery was full, so Will was rushed to the NICU and we had a cascade of “worst case scenarios” thrown at us, including me being told I couldn’t hold him or nurse him. We had 20-22 hours of doom and gloom - everything from suspecting a perforated bowel, to a life threatening blood infection. The NICU lactation consultant was our voice of reason, but not our primary provider. She asked how fast labor happened (fast) and said that the “vomit” looked more like amniotic fluid mixed with colostrum. She suspected he had “water in the lungs” and in his tummy because things progressed so quickly that he didn’t get enough good squeezes and that he swallowed fluid on his way out (my water didn’t break until I started pushing).
She pushed to get the NICU doctor to let him breastfeed after they completed the X-ray and MRI to confirm he didn’t have a perforated bowel. We still had to wait a minimum of 48 hours, but protocol said 72 hours, to ensure there was not a life threatening blood infection. Thankfully, there wasn’t and we did get to go home at 4 days old. The NICU restrictions for my otherwise healthy baby, were really difficult. I wasn’t allowed to hold him, and while I would have preferred to nurse him and let him linger at the breast as long as he wanted - they “needed” him back in the crib. I’m so thankful they were able to provide such great care and I know the NICU is life or death for so many families - but I would have liked to see more individualized care because the mandatory times, tests, and protocols were very difficult for an otherwise healthy baby. This took a huge toll on my emotional wellbeing. We couldn’t have visitors, I couldn’t hold my baby, I didn’t have a recovery area in his room so I spent a lot of time going back and forth while trying to manage my own recovery and care for him. And then the IV sugars and fluids he received required extra tests and requirements about how much milk my days old baby should be taking and demands to supplement with formula before they would let us leave and it was all so much to handle.
My postpartum period for those first few weeks left me with a lot of dark feelings, fears, loneliness, and so much crying. I didn’t know what I needed to feel supported and well, but we had spent so much time preparing for a VBAC that we didn’t know what to do postpartum and I wish we had been more prepared. The postpartum period was hard on both my husband and I as parents, and also on our bigger kids. We all had a difficult time adjusting, and I just wish I had known how to make that easier.
——
My doula was such a valued member of our team. I wish that they were available to everyone, but especially birthing people who are most at risk of birth complications (because of systemic racism, because of other factors, etc), who have more “difficult’ births (like my VBAC, which many hospitals would consider difficult), or really - everyone. Our doula - Alicia - made a tremendous difference and helped my husband almost as much as she helped me. He was able to stay focused on what I needed, and when I veered out of my zone she helped guide me back into focus. She knew how to help get me into positions favorable to getting Will to move down. I really think that I was so lucky to have the best team on board for me. I also had an amazing nurse - Jenny was a midwife in South Africa and the UK, and is now a nurse at the hospital where Will was delivered. Her experience was so important in helping me achieve the VBAC. She helped guide me, and trusted my body. (For my first delivery, my nurse was the least helpful person in the room. Much of her advice was now what I know was the opposite of what I should have been doing to move Jack into a good position. And it was Jack’s delivery which set me up for a cesarean with my middle child Ava and my midwife team. They were so much better to me as a patient that the OB group I used with Jack and Ava. They informed me and helped me get all I needed to make a decision. They told me what they would choose and why, but that I could also do B for x reasons, or C for y reasons. They were the epitome of personalized care. And they never let me to believe that they doubted me one bit. The “truth” I shared in an earlier question about intuition. Trust your intuition about your care team. I wish I had trusted myself when I had fears with Ava’s pregnancy about my care team. I shoved those fears down when I should have listened.
Each of my deliveries were different experiences all together. Jack, a tv-style hospital delivery with an OB, plus shoulder dystocia and an unsupported and abandoned breastfeeding journey. Ava, a scheduled cesarean because my OB told me we’d be risking our lives if we tried a vaginal delivery and an amazing breastfeeding relationship (26 months) that came relatively easily with awesome weight gain. Will, an empowering VBAC, scary NICU stay, and still going strong with breastfeeding at a year but a much slower weight gain despite him being my biggest baby at birth (he’s now the smallest of the three were at a year old!) All three kiddos look very much like OUR CHILDREN but are such different infant experiences. It just goes to show that you think you know how to do this but each baby is different. It’s comfortable, yet new, and it’s confusing at times. But it’s really lovely and I am so glad that our family is complete.